Bone and Dental Health in Pregnancy: Tips for Before and After Birth


Bone and Dental Health in Pregnancy: Tips for Before and After Birth
 By Inventive Minds Kidz Academy
By Inventive Minds Kidz Academy
 Added Wed, May 13 2026
Added Wed, May 13 2026
 By Inventive Minds Kidz Academy
By Inventive Minds Kidz Academy
Added Wed, May 13 2026
Hey, Thanks For Subscribing!
Please check for a confirmation message and ensure you add us to a safe email list.
If you don't see a message in the next five minutes, check your spam or junk folders and mark our emails safe for next time.
See you soon!
Duplicate Email Found!
Well this is embarrassing... It looks like is already registered.
We have just sent an email to that address with a link to manage the subscription with us. If you don't see a message in the next five minutes, check the spam or junk folders, it's definitely there.
See you soon!
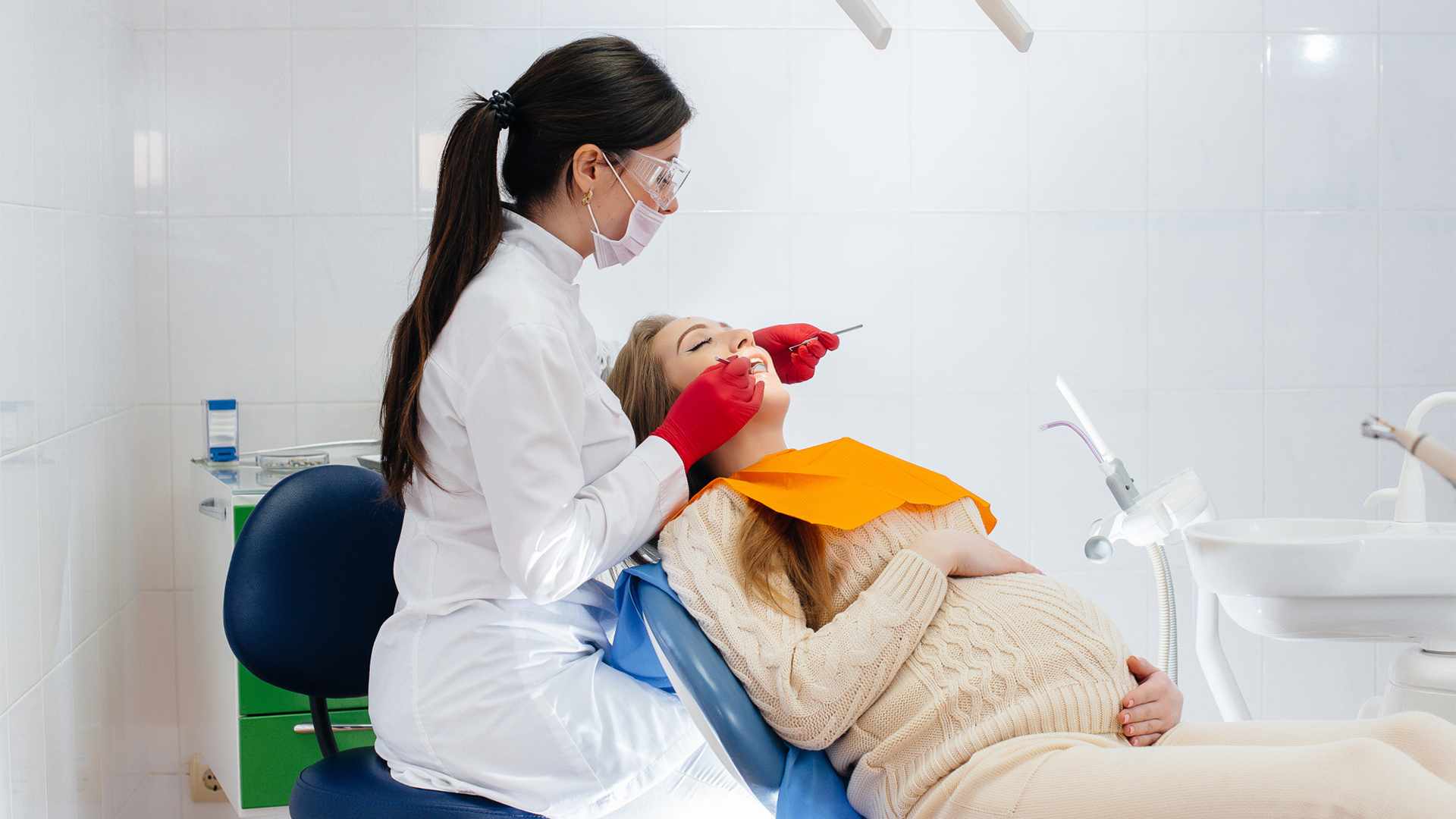
Pregnancy, birth giving and breastfeeding are most transformative periods in a woman’s life, both mentally and physiologically. Meaning that mother’s body goes through significant changes in how it works during these periods, so it will be able to support development of child. These changes not only involve hormonal changes, mental difficulties, circulatory system and metabolic system but also musculoskeletal system. Bones and muscles undergo substantial adaptations to meet the increased demand for calcium, phosphorus and other required essential minerals for fetal bone formation and milk production. Taking the right supplements and Keeping bones healthy in these periods require careful attention as the consequences of deficiency may be long-term for both mother and the child.
The physiological impact of pregnancy and breastfeeding on bone health
During pregnancy, the developing fetus requires 30 grams of calcium on average for mineralization of it’s skeleton. The need for calcium is especially high during the third trimester. The mother’s body adapts to this high demand by enhancing calcium absorption in the intestines and releasing calcium from the maternal bones. According to Williams Textbook of Obstetrics, “maternal calcium absorption increases significantly in the second half of pregnancy to meet fetal mineral demands.” The increase in bone resorption is mediated by elevated levels of parathyroid hormone-related peptide (PTHrP) and other hormones like estrogen and calcitonin, which affect bone remodeling processes.
While this adaptive mechanism makes sure that baby’s bones are adequately developed, it places a considerable stress on the mother’s skeletal system. If the maternal diet does not provide sufficient calcium, her body compensates by drawing calcium from the bones.
Breastfeeding further exacerbates mineral demands, as approximately 200-300 mg of calcium is transferred daily to breast milk (approximately 100gr of calcium in the first year). During lactation, estrogen levels also remain low, reducing bone formation and increasing bone resorption to mobilize calcium stores. These physiological changes can lead to bone loss in the mother, which is typically restored post-weaning. Williams Textbook of Obstetrics states, “Lactation-induced bone loss is generally transient and is largely restored within 6-12 months post-weaning.” However, inadequate dietary intake or supplementation of key nutrients during this period can have lasting consequences.
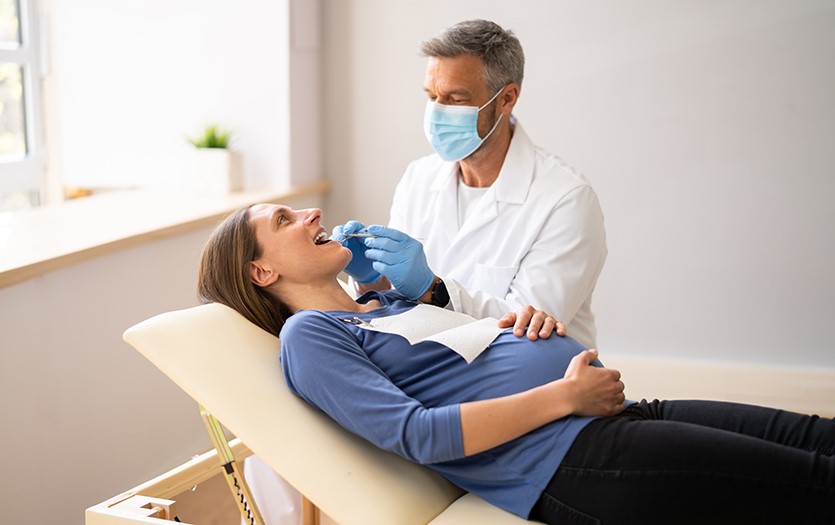
Dental Health During Pregnancy
Pregnancy-related hormonal changes also affect oral health. Elevated progesterone and estrogen levels can increase the risk of gingivitis, periodontal disease, and dental caries. According to Williams Textbook of Obstetrics, “Pregnancy-associated gingivitis affects up to 70% of pregnant women, characterized by gum swelling, redness, and bleeding.” Additionally, morning sickness and acid reflux can lead to increased enamel erosion, further compromising dental health.
Periodontal disease during pregnancy has been associated with adverse pregnancy outcomes, including preterm birth and low birth weight. Poor oral health can also affect postpartum well-being, making dental care an essential component of maternal health. Preventive measures, including routine dental checkups, proper oral hygiene, and dietary modifications, can help mitigate these risks.
Key nutrients for bone health during and after pregnancy
Calcium is the primary mineral required for fetal bone formation and maternal bone maintenance. During pregnancy the recommended daily intake of calcium increases to about 1,000 mg/day, with a higher requirement during the third trimester (up to 1,200 mg/day). After birth, calcium requirement remains high for lactating women, with recommendations ranging from 1,000 to 1,200 mg/day.
Another nutrient, although not mineral, is Vitamin D3. Vitamin D3 is crucial for calcium absorption and bone mineralization. The RDA for vitamin D is 600 IU/day during pregnancy, but higher doses (up to 4,000 IU/day) may be required in deficient individuals. Sunlight exposure and fortified foods contribute to vitamin D levels, but supplementation is often recommended, especially in regions with limited sunlight. Deficiency during pregnancy is associated with reduced fetal bone density, reduced maternal bone density and an increased risk of neonatal rickets. Williams Textbook of Obstetrics mentions that “Vitamin D deficiency in pregnancy is associated with reduced fetal bone density and increased risk of maternal osteopenia.”
The RDA for vitamin D3 for breastfeeding women is also around 600 IU/day. Because the vitamin D3 is not adequately secreted to breast milk, vitamin D3 supplements are also recommended for newborns.
Magnesium plays a role in bone matrix formation and calcium metabolism. Zinc is essential for bone growth and remodeling. Phosphorus works synergistically with calcium in bone mineralization and also vitamin K2 regulates osteocalcin, a protein involved in bone formation. Adequate intake of these nutrients is vital for maintaining bone health. Deficiencies in these minerals can also impair fetal skeletal development and exacerbate maternal bone loss.
Consequences of nutrient deficiency on bone health
Inadequate intake of calcium, vitamin D, and other above-mentioned bone-supporting nutrients can lead to maternal osteopenia or osteoporosis, increasing the risk of fractures. Williams Textbook of Obstetrics reports that “pregnancy-associated osteoporosis, although rare, can result in severe vertebral fractures and chronic pain, particularly in women with low body mass index or multiple pregnancies.”. Also, many women experience musculoskeletal pain in the first few months postpartum, often attributed to hormonal changes, physical strains and transient bone loss. Nutrient deficiencies can exacerbate these symptoms, delaying recovery and impacting mother’s quality of life.
Oral health complications due to poor nutrition include tooth decay, gum disease, and enamel erosion. Severe periodontal disease has been associated with systemic inflammation, potentially affecting pregnancy outcomes
For the baby, inadequate maternal intake of these essential nutrients during pregnancy and breastfeeding can negatively affect bone mineralization, leading to a higher risk of bone deformities and fractures in the early years of life. Furthermore, the long-term bone health of the infant may also be compromised, as proper bone development in infancy and childhood is dependent on maternal nutrient status during pregnancy and breastfeeding.
Oral hygiene, Dietary changes and supplemental recommendations
Regular dental checkups, daily brushing with fluoride toothpaste, flossing, and reducing sugary foods can help prevent pregnancy-associated dental issues. Dentists may also recommend antimicrobial mouthwashes to reduce bacterial plaque buildup.
Dietary modifications are important for maintaining bone health during pregnancy and breastfeeding. A diet rich in calcium, vitamin D, and other bone-supporting nutrients that we have mentioned may help meet increased physiological demands. Dairy products such as milk, cheese, and yogurt are excellent sources of calcium, while fatty fish (e.g., salmon, mackerel) and egg yolks provide vitamin D. Fortified foods, including cereals and plant-based milk alternatives can also enhance nutrient intake. Leafy greens such as kale and spinach, nuts, seeds, and legumes contribute magnesium and phosphorus. For vitamin K2, fermented foods like natto and certain cheeses are beneficial.
All that said, having a greatly balanced diet is too far from reach most of the times, and even if it was in reach, it might not be enough. That’s where supplements come in. Calcium and vitamin D3 supplements are often empirically recommended by obstetricians. Zinc and magnesium supplements may also be recommended, depending on dietary intake and individual needs.

Authored by:
Dr. Alireza Sarmadi
Family Physician
References:
- Williams textbook of obstetrics 26e
- Rood, J. M., et al. (2012). Calcium and bone metabolism during pregnancy and lactation. Nutrition Reviews, 70(2), 89-101.
- Vatanparast, H., et al. (2019). Bone health in pregnancy and lactation. The Journal of Clinical Endocrinology & Metabolism, 104(9), 4207-4215.
- Ross, A. C., et al. (2011). The 2011 Dietary Reference Intakes for calcium and vitamin D. The Journal of Clinical Endocrinology & Metabolism, 96(1), 53-58.
- Holick, M. F. (2007). Vitamin D Deficiency. *The New England Journal of Medicine, 357*(3), 266-281.
- Prentice, A. (2003). Micronutrients and the Bone Mineral Content of the Mother, Fetus, and Newborn. *The Journal of Nutrition, 133*(5), 1693S-1699S.
- Weaver, C. M., & Heaney, R. P. (2006). Calcium. In *Modern Nutrition in Health and Disease* (10th ed., pp. 194-210). Lippincott Williams & Wilkins.
- World Health Organization (WHO). (2013). Calcium Supplementation During Pregnancy to Reduce the Risk of Pre-Eclampsia. *WHO Guidelines*.
Pregnancy, birth giving and breastfeeding are most transformative periods in a woman’s life, both mentally and physiologically. Meaning that mother’s body goes through significant changes in how it works during these periods, so it will be able to support development of child. These changes not only involve hormonal changes, mental difficulties, circulatory system and metabolic system but also musculoskeletal system. Bones and muscles undergo substantial adaptations to meet the increased demand for calcium, phosphorus and other required essential minerals for fetal bone formation and milk production. Taking the right supplements and Keeping bones healthy in these periods require careful attention as the consequences of deficiency may be long-term for both mother and the child.
The physiological impact of pregnancy and breastfeeding on bone health
During pregnancy, the developing fetus requires 30 grams of calcium on average for mineralization of it’s skeleton. The need for calcium is especially high during the third trimester. The mother’s body adapts to this high demand by enhancing calcium absorption in the intestines and releasing calcium from the maternal bones. According to Williams Textbook of Obstetrics, “maternal calcium absorption increases significantly in the second half of pregnancy to meet fetal mineral demands.” The increase in bone resorption is mediated by elevated levels of parathyroid hormone-related peptide (PTHrP) and other hormones like estrogen and calcitonin, which affect bone remodeling processes.
While this adaptive mechanism makes sure that baby’s bones are adequately developed, it places a considerable stress on the mother’s skeletal system. If the maternal diet does not provide sufficient calcium, her body compensates by drawing calcium from the bones.
Breastfeeding further exacerbates mineral demands, as approximately 200-300 mg of calcium is transferred daily to breast milk (approximately 100gr of calcium in the first year). During lactation, estrogen levels also remain low, reducing bone formation and increasing bone resorption to mobilize calcium stores. These physiological changes can lead to bone loss in the mother, which is typically restored post-weaning. Williams Textbook of Obstetrics states, “Lactation-induced bone loss is generally transient and is largely restored within 6-12 months post-weaning.” However, inadequate dietary intake or supplementation of key nutrients during this period can have lasting consequences.

Dental Health During Pregnancy
Pregnancy-related hormonal changes also affect oral health. Elevated progesterone and estrogen levels can increase the risk of gingivitis, periodontal disease, and dental caries. According to Williams Textbook of Obstetrics, “Pregnancy-associated gingivitis affects up to 70% of pregnant women, characterized by gum swelling, redness, and bleeding.” Additionally, morning sickness and acid reflux can lead to increased enamel erosion, further compromising dental health.
Periodontal disease during pregnancy has been associated with adverse pregnancy outcomes, including preterm birth and low birth weight. Poor oral health can also affect postpartum well-being, making dental care an essential component of maternal health. Preventive measures, including routine dental checkups, proper oral hygiene, and dietary modifications, can help mitigate these risks.

Key nutrients for bone health during and after pregnancy
Calcium is the primary mineral required for fetal bone formation and maternal bone maintenance. During pregnancy the recommended daily intake of calcium increases to about 1,000 mg/day, with a higher requirement during the third trimester (up to 1,200 mg/day). After birth, calcium requirement remains high for lactating women, with recommendations ranging from 1,000 to 1,200 mg/day.
Another nutrient, although not mineral, is Vitamin D3. Vitamin D3 is crucial for calcium absorption and bone mineralization. The RDA for vitamin D is 600 IU/day during pregnancy, but higher doses (up to 4,000 IU/day) may be required in deficient individuals. Sunlight exposure and fortified foods contribute to vitamin D levels, but supplementation is often recommended, especially in regions with limited sunlight. Deficiency during pregnancy is associated with reduced fetal bone density, reduced maternal bone density and an increased risk of neonatal rickets. Williams Textbook of Obstetrics mentions that “Vitamin D deficiency in pregnancy is associated with reduced fetal bone density and increased risk of maternal osteopenia.”
The RDA for vitamin D3 for breastfeeding women is also around 600 IU/day. Because the vitamin D3 is not adequately secreted to breast milk, vitamin D3 supplements are also recommended for newborns.
Magnesium plays a role in bone matrix formation and calcium metabolism. Zinc is essential for bone growth and remodeling. Phosphorus works synergistically with calcium in bone mineralization and also vitamin K2 regulates osteocalcin, a protein involved in bone formation. Adequate intake of these nutrients is vital for maintaining bone health. Deficiencies in these minerals can also impair fetal skeletal development and exacerbate maternal bone loss.
Consequences of nutrient deficiency on bone health
Inadequate intake of calcium, vitamin D, and other above-mentioned bone-supporting nutrients can lead to maternal osteopenia or osteoporosis, increasing the risk of fractures. Williams Textbook of Obstetrics reports that “pregnancy-associated osteoporosis, although rare, can result in severe vertebral fractures and chronic pain, particularly in women with low body mass index or multiple pregnancies.”. Also, many women experience musculoskeletal pain in the first few months postpartum, often attributed to hormonal changes, physical strains and transient bone loss. Nutrient deficiencies can exacerbate these symptoms, delaying recovery and impacting mother’s quality of life.
Oral health complications due to poor nutrition include tooth decay, gum disease, and enamel erosion. Severe periodontal disease has been associated with systemic inflammation, potentially affecting pregnancy outcomes
For the baby, inadequate maternal intake of these essential nutrients during pregnancy and breastfeeding can negatively affect bone mineralization, leading to a higher risk of bone deformities and fractures in the early years of life. Furthermore, the long-term bone health of the infant may also be compromised, as proper bone development in infancy and childhood is dependent on maternal nutrient status during pregnancy and breastfeeding.
Oral hygiene, Dietary changes and supplemental recommendations
Regular dental checkups, daily brushing with fluoride toothpaste, flossing, and reducing sugary foods can help prevent pregnancy-associated dental issues. Dentists may also recommend antimicrobial mouthwashes to reduce bacterial plaque buildup.
Dietary modifications are important for maintaining bone health during pregnancy and breastfeeding. A diet rich in calcium, vitamin D, and other bone-supporting nutrients that we have mentioned may help meet increased physiological demands. Dairy products such as milk, cheese, and yogurt are excellent sources of calcium, while fatty fish (e.g., salmon, mackerel) and egg yolks provide vitamin D. Fortified foods, including cereals and plant-based milk alternatives can also enhance nutrient intake. Leafy greens such as kale and spinach, nuts, seeds, and legumes contribute magnesium and phosphorus. For vitamin K2, fermented foods like natto and certain cheeses are beneficial.
All that said, having a greatly balanced diet is too far from reach most of the times, and even if it was in reach, it might not be enough. That’s where supplements come in. Calcium and vitamin D3 supplements are often empirically recommended by obstetricians. Zinc and magnesium supplements may also be recommended, depending on dietary intake and individual needs.

Authored by:
Dr. Alireza Sarmadi
Family Physician
References:
- Williams textbook of obstetrics 26e
- Rood, J. M., et al. (2012). Calcium and bone metabolism during pregnancy and lactation. Nutrition Reviews, 70(2), 89-101.
- Vatanparast, H., et al. (2019). Bone health in pregnancy and lactation. The Journal of Clinical Endocrinology & Metabolism, 104(9), 4207-4215.
- Ross, A. C., et al. (2011). The 2011 Dietary Reference Intakes for calcium and vitamin D. The Journal of Clinical Endocrinology & Metabolism, 96(1), 53-58.
- Holick, M. F. (2007). Vitamin D Deficiency. *The New England Journal of Medicine, 357*(3), 266-281.
- Prentice, A. (2003). Micronutrients and the Bone Mineral Content of the Mother, Fetus, and Newborn. *The Journal of Nutrition, 133*(5), 1693S-1699S.
- Weaver, C. M., & Heaney, R. P. (2006). Calcium. In *Modern Nutrition in Health and Disease* (10th ed., pp. 194-210). Lippincott Williams & Wilkins.
- World Health Organization (WHO). (2013). Calcium Supplementation During Pregnancy to Reduce the Risk of Pre-Eclampsia. *WHO Guidelines*.
Most Talked About Posts
You May Also Like
Staff Picks
Now Trending
Our Newsletter
Duplicate Email Found!
Well this is embarrassing... It looks like is already registered.
We have just sent an email to that address with a link to manage the subscription with us. If you don't see a message in the next five minutes, check the spam or junk folders, it's definitely there.
See you soon!
Join Our Newsletter
Hey, Thanks For Subscribing!
Please check for a confirmation message and ensure you add us to a safe email list.
If you don't see a message in the next five minutes, check your spam or junk folders and mark our emails safe for next time.
See you soon!
Duplicate Email Found!
Well this is embarrassing... It looks like is already registered.
We have just sent an email to that address with a link to manage the subscription with us. If you don't see a message in the next five minutes, check the spam or junk folders, it's definitely there.
See you soon!










